QA on Vaccines
From my Facebook Messages:
Dr Hinson,
Feel free to not answer this question since this is your personal facebook, but I thought I’d give it a try.
I’ve only immunized one of my children, and have remained undecided for the others because of the controversy of vaccines’ effectiveness/dangers. In my limited experience with you as a Dr, you seemed to be in the middle of the road between conventional medicine and natural alternatives, so I’m interested in your opinion. Which vaccines, if any, do you think are necessary?
Thanks in advance. I hope things are going well for you with your plans of a new practice!
JS
PS. We just moved, and the few Drs in our area so far seem to be seriously conventional only, ie: antibiotics absolutely necessary for ear infections, the nurse looked at me like I had 3 heads because I didn’t want the flu shot (after I told her I’d already had the flu this year), and I just found out my Dr will no longer see me for prenatal care because I’d like a home birth with a midwife. All that to say, we miss you guys! You guys rocked.
I think there is little reason to worry about any of the vaccines that are out there. Are they risk-free? No. There are always risks (mostly in the form of allergic reactions). But the risks are so low as to be less than the chance of getting sick from the diseases they protect you from. (Unfortunately, this is more and more the case thanks to the unwarranted controversies out there that have affected vaccine rates.) For example, the polio shot. Polio pretty much no longer exists here in the US. So, you could ask, why bother with the shot? Well, it is almost as unheard of to have a reaction to it. And, there is certainly the possibility that a kid might grow up to be the wonderful person that decides to join the Peace Corp and go work in sub-Saharan Africa where the disease persists. And then that apple-of-any-mother’s eye might bring it back and reintroduce it here. So, as unlikely as that might seem, it is more likely than a problem from the shot.
Now, the polio shot also demonstrates another important facet of the immunization debate–public vs personal benefit. If a child born today is not vaccinated at all, the truth is, there is not a huge risk these days. However, I can only say that because of the vaccination program. If every child in your child’s daycare or school is vaccinated, and your child never leaves the island, the risk would be very low, and one could argue against the need to vaccinate. BUT, what if everyone came to that same conclusion? There is a concept known as herd immunity. As long as a certain percentage of the population is vaccinated, then, we don’t have as much to worry about as a public health issue, and this huge public health advantage is easily overlooked these days, as we have gotten so use to low-to-zero rates of some of the diseases involved.
That said, to answer you question, what vaccines are most important to personal health these days? That is, if not vaccinated, which diseases are most likely to greatly affect a kid, i.e., hospitalize them, or even lead to something worse?
I would rank them like this (and this is just opinion, unencumbered by science, stats or the CDC):
1. flu
2. HIB*
3. Pneumococcal*
4. Rotavirus
5. Pertussis
6. Measles
7. Mumps
8. Tetanus
9. …the rest.
Flu? Seriously? Yep. If you simply look at stats, that is the infection most likely to cause death! HIB and pneumococcal are starred because this list is age dependent. If you are asking about a 6 or 8 year old, these are less important because these are common bacteria. They’re everywhere. They cause the vast majority of ear infections, sinus infections, pneumonias, and even meningitis cases in kids under 5. And, as such, they are very pertinent vaccines to be given to an under-2. But, by the time you’re 5 or 6, your immune system has seen the germs so much as to have created its own native immunity. Another way of looking at this is, you are much, much more likely to hospitalize a 1.5 yr old with pneumonia than we are a 10 year old with it.
So, there. Probably more than you wanted to hear. But the vaccine program is extremely important to our society. We are a generation or two removed from when everyone knew someone paralyzed from polio, or made infertile by mumps or born with horrible birth defects due to rubella. We are removed enough that all of that is easily forgotten.
GH
Not too much info. I soak this stuff up. Thanks so much for taking the time. You’ve possibly convinced me…and if that’s the case, my sister who is a nurse thanks you!
JS
I’m going to give you one more bit of info (that you did not ask for). Toxins. Heavy metals. Mercury. Etc. Do you realize you would have to get 75 flu shots at once to get the amount of mercury (in a different, less-toxic form, no less) to equal the amount you would get from eating a serving of swordfish? (And, to make it more local, just 4 tiny bay scallops have the amount of mercury that you see in one flu shot.)
Like everything else that is manufactured–plastics, apple skin wax, shampoo–vaccines have “industrial” ingredients. But so does the real world. You cannot avoid this stuff; it’s in the air we breathe, the water we drink, even on the shelf at Annye’s. It’s a testimony to our bodies’ ability to handle all of this stuff that we’re not all sick all the time. And yet, as our environment has become more and more saturated with stuff like this, our life expectancy has continued to climb.
Now, does that mean you should bathe a kid in pesticide and feed them nothing but processed foods, heated in plastic? No. Of course not. But, when there is measurable benefit to something, e.g., vaccines, it means there’s no reason to be overly afraid of it.
Okay. I’m done. Stepping down from the pulpit to go turn this in to a blog post. Hmmm. Certainly went on long enough about it…
GH
Haha, you should. Just copy and paste. I didn’t realize that about the mercury until I was sitting in your office last year and saw the chart comparison. I was really surprised!
I suppose I tend to look at the flip side. I think of all the pesticides, processed foods, prescription drugs, and look at all the food allergies, autoimmune disease, chronic conditions that seem to be absolutely everywhere. Yes we live longer but at what quality? Is it just the drugs that keep our bodies ticking but really we are unhealthier than ever?
JS
Again, without researching the science to back this up (if there is any), I would say that we are more used to good health, so simpler things like food intolerances or arthralgias are now more likely to be complaints. If, say fifty years ago, you could barely walk due to polio or were 40 years old and going blind from uncontrolled diabetes, you probably were not going to complain much about your “rheumatism.”
That said, there is still every reason for vigilance. Just because meds might be able to extend your life, doesn’t mean it should be one of misery. I do not believe meds are as good at extending one’s life as getting out of the chair, moving, and eating less food, but better foods (that are less processed and more local).
This is where modern life and its techno advances are a blessing and a curse. There are more and more options for recreation and exercise; but it is a lot easier to never get out of a chair these days. Given transportation systems and advanced agri techniques, it easier to eat better (we certainly have less to fear for from famine); but at the same time, the same technologies have made it much easier to eat poorly too.
The older I get, I think these two things are more important than anything you can buy on a shelf (e.g, supplements, vitamins, natural meds, cleanses, etc.) or anything ordered on a prescription pad!
GH
Interesting point at the beginning…hadn’t thought if that. Love this convo.
JS
A healthy addiction
It’s only been a week, and I am hooked. Go to bed thinking about it. Wake up thinking about it. Trust it to watch over me while I sleep. Listen to it when it tells me to eat right and exercise. Beam with pride when it rewards me for losing 5 lbs (in one week, by the way). Allow it to help me make healthy choices while living in a hotel room and eating out every meal. I am a Fitbit user.
In case you’re unfamiliar with it, the Fitbit One is a pedometer. Shaped like a cross between a guitar pick and a baby carrot, it is made to sit in your pocket, connect imperceptibly to your smartphone or computer, and count your steps. In so doing, along with you actively entering data like what you eat, your age and weight, and your fitness goals, it becomes a pocket fitness instructor. Additionally, if you wear it on your wrist at night, it also monitors your sleep, counting how long you sleep, how often you wake, and how efficient your sleep is. It’s made me go to bed earlier, so as to not disappoint it.
The company makes several devices, including a wifi-enabled scale that, once sets up, know you when you step on it, and automatically sends your weight and percent body fat to the device. Lastly, the company hosts online groups of users, turn the process of getting in to shape into a social game. We need a Nantucket Fitbit Users Group. Anyone else out there?
I’m in talks with the company about becoming a wholesaler so I can supply them to patients in my next practice. The little device (at $99), by enabling and encouraging a healthy lifestyle, is likely more valuable than any pill I will prescribe.
Survey: Grocery Shopping on Nantucket.
The barriers and motivators for shopping for food downtown.
Introduction.
Caffeinated, Inc., an advertising and branding firm based on Nantucket recently conducted a survey of 466 individuals regarding the habits and attitudes around grocery shopping on the island. This report represents a broad executive summary of the data and findings. More detailed data is available upon request.
The situation.
Choice has never been a watchword for grocery shoppers on Nantucket. The standards at the current Stop & Shop are low compared to offerings off island, and the quality and selection at the former Grand Union had been universally viewed as worse than the Stop & Shop. There are some high quality offerings on island in Annye’s and Bartlett Farm, but neither of these stores provides a complete “supermarket” offering, so they are viewed largely as specialty grocery retailers.
About our respondents.
466 unique individuals took the survey online over a three week period in late November and early december. Measures were taken to ensure that individuals could not take the survey more than once. Over one quarter of the respondents were seasonal residents or visitors. Half of the respondents live close to town, largely in the mid-island area, close to the existing Stop & Shop. 43% of those who responded have an income in excess of $75,000, with 29% over $100,000 annually.
About the survey.
The survey itself can be viewed here: http://caffeinated.wufoo.com/forms/nantucket-grocery-shopping-survey/. This survey came in the wake of an overwhelming public sentiment that a CVS was not right for the downtown Nantucket. Once the community had explained what it did not want, it was time to understand what it did want and would support. This survey provides some insight into those questions.
Some key findings include:
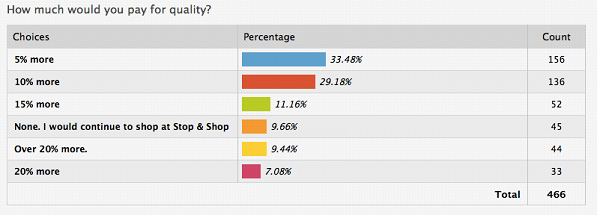
Quality trumps price for year-round shoppers.
While the majority of year-rounders strike a balance between quality and price, well over one third put quality first. This represents a potential opportunity for a higher-end grocery downtown.
(Year round residents)
There is room for higher quality and price in the marketplace.
Roughly a third of respondents would pay a 10% premium for better quality over Stop & Shop (which is already estimated to cost 15% more than the mainland. And one quarter would pay over 15%.
In fact, over 70% of those surveyed said they would be likely to shop downtown in the Summer if the grocer there had better quality than Stop & Shop. 85% were likely or highly likely to shop downtown in the face of better quality in the winter, which represents a large portion of Stop & Shop’s core business. Only 8.8% of respondents said they would continue to shop in the mid-island under such circumstances.
Fresh produce, meats would be a welcome addition for year-round shoppers.
Among 86% of year-round residents, superior produce is seen as a major motivator to shop downtown, with superior quality meats begin second at 80.6%
(Year round residents only)
The parking situation is complicated.
80% of respondents said that ample free parking would get them to drive into the downtown area to shop there, but very few of them felt that way about ample paid parking (25%). When asked how much they would be willing to pay for parking over half said they would not be willing at all.
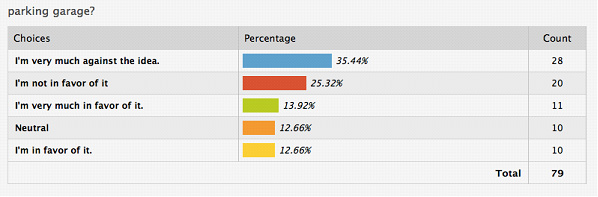
Year-round residents were against a parking garage on the site by a ratio of two to one, with 20% of respondents neutral on the subject. Seasonal residents were even more adamantly opposed:
(Seasonal residents)
Additional information and comparative data is available from this survey. Please contact Grant Sanders of Caffeinated, Inc (grant@caffeinated.com) for information.
© Copyright 2012 Caffeinated, Inc. All rights reserved.
Exercise for Satiety

It’s a new year. I’m planning my office. And, recognizing that sitting is the new smoking–a recent study showed that as many as 1 in 10 deaths are secondary to prolonged inactivity–it is time to get serious about exercise again. In planning my office, I’m considering getting a treadmill with a work desk attached to it. Have you seen these? It would take up enough space so as to make it hard to not get on it throughout the day. For example, this one. I also just ordered a pair of Fitbits. You have probably heard about these little electronic pedometers that sync with your smart phone and track your numbers, e.g., steps, miles, calories burned, etc. I’m excited to try out the gamification that comes with them. You can set up a network of friends and compete. Being a naturally competitive person, with a wife that works out most days, that should be good for me (to have to live up to her standards). And I’m excited to extend this network to other friends and patients. A challenge (first, I have to see if I can avoid embarrassment being compared to Amy).
A blog post in the NY Times this past week discussed the effect of exercise on appetite. Most people recognize that exercise is not, in itself, a good way to lose weight. In fact, sometimes it causes you to gain weight. Appetite causes a spike in ghrelin levels, a hormone that stimulates hunger. And if you give in to this, you can easily defeat your exercise. Classic scenario, you set the alarm, wake up early, go out for a run. On the way home, proud that you displayed such disclipine, you stop at the Flake on the way home, and get a single donut and a cup of coffee, and ingest more calories than you just burned!
The post summed up two recent research studies, however, that showed that, with time, certain types of exercise increases the levels of other hormones, the as yet not well understood satiety hormones that mute the effect of ghrelin. In short, persistent, moderate exercise (the equivalence of a brief, brisk jog), showed a suppression in their appetite, whereas those that only walked did not suppress their appetites.
The post quoted the researcher: Exercise “improves the body’s ability to judge the amount of calories consumed and to adjust for that afterward.”
A New Therapy That is Difficile to Swallow

Imagine the following. A tube is placed down a nostril, snaked into and through your stomach, right to the start of your intestines. Then someone else’s stool is pumped in to the tube and down your throat.
And if you’re suffering from a “C-diff” infection, trust me, the day has come when you’ll be begging for it. You can ask someone who has experienced it, or just ask an experienced nurse, about what it is like to suffer through the severe diarrhea that comes from an infection by the bacteria Clostridium difficile. It is severe, non-stop, and often life-threatening. It generally only happens when the gut has been robbed of its normal flora, the bacteria that is supposed to be there to compete with bad guys like C-diff (and a good reason to run whenever you hear anyone talk about a “colon cleanse,” a clean colon is an unhealthy colon!).
A C-diff infection is notoriously hard to treat, sometimes requiring months of a potentially toxic IV antibiotic (Vancomycin). But a new study seems to verify an old treatment. We can treat the infection by doing a fecal transplant, essentially replacing the normal flora that should be there. I have to say, when I first read about this treatment, my immediate response was “No Shit!” It makes sense though.
Donor stool is screened for parasites and other serious infections, diluted and strained, and is then introduced in to the patient. (Now, to be fair, in Europe studies have been performed with the nasogastric tube as described above, but in the US, studies have been done via colonscopy.) The study linked to above was stopped early because it was so successful as to mean it would be unethical to continue the control arm. The treatment was 94% effective. Of 16 transplant patients, 13 were cured on their first infusion, and two more on a repeat round. In the two drug arms, the rates were 31 percent in the vancomycin-only group (4 of 13) and 23 percent (3 of 13) in the group receiving vancomycin plus lavage. That’s amazing.
In science, everything always needs to be repeated, and every endorsement is always hedged — but really, this was a rousing success. As an accompanying editorial says:
The study is an important confirmation of the efficacy of (fecal microbiota transplantation) for recurrent C. difficile infection… The results … represent a clear precedent in which planned therapeutic manipulation of the human intestinal microbiota can lead to demonstrable, clinically important benefits, thereby bringing FMT to the mainstream of modern, evidence-based medical practice. (It) will encourage and facilitate the design of similar trials of intestinal microbiota therapy for other indications, such as inflammatory bowel disease, irritable bowel syndrome, prevention of colorectal carcinoma, and metabolic disorders, to name just a few.
Given the Yuck factor, once we can meet the demand for the procedure as is, the next goal will be to create a synthetic stool, grow in cultures the bacteria needed and suspend them in some sort of benign slushy. NPR’s Shots health blog has a great interview with the Canadian team who came up with the synthetic substitute, amusingly dubbed “RePOOPulate.”
Kodak, Instagram and Healthcare

Dr. Rob Lamberts is a new friend of mine. (I’ve never actually met him, but with Facebook and Twitter and the like, you no longer to know someone to know someone, right?)
He is a Med-Peds physician in Augusta, GA, who is also rebounding from burn out (my diagnosis, not his).
Looking through his blog, I found an entry from last fall that, I think, speaks a lot of truth about the impending implosion of our health care system. At a time when costs are escalating, and quality is falling, and more and more people are going to make use of the health care system given the well-meaning, but ultimately misguided policies of the Affordable Care Act (I’ll go in to that more at a later date), something has to change. This industry has to evolve, or it risks becoming the Kodak of the first part of this century.
Kodak was, at one point, the consummate American success story, dominating its market like few others. In 1976, it had a 90% market share of film, as well as 80% of cameras sold in the US. Kodak Park, the property at the center of manufacturing once employed 29,000 employees, with its own fire company, rail system, water treatment plant, and continuously staffed medical facility.
Fast-forward to 2012, and the picture changes dramatically. In a single year, Kodak declared chapter 11 bankruptcy, received a warning from the New York Stock Exchange that its stock was below $1/share for long enough that it was at risk of being delisted, announced it is no longer making digital cameras so as to focus on its core business: printing, and then a few weeks ago announced it was no longer making inkjet printers. The job force in Rochester alone has gone down by nearly 90%, to an estimated 7200 employees.
Adding pain for former Kodak fans was the announcement in April of this year that Facebook was buying the photo sharing company Instagram (which employed 13 people at the time) for an estimated $1 Billion.
I remember reading that at the time of their bankruptcy hearings, a judge placed a value of $525 million on the assets (primarily patents) of the company. And here the app, whose sole purpose is to take a photo that pales in comparison with the quality of a photo taken on kodak film, then to apply a filter to it, making it look like a photo taken on old, outdated film, was purchased for almost twice that amount!
…the success of Instagram at the expense of the wonderful folks up in Rochester happened because Kodak had too much at stake to embrace a disruptive technology that spelled doom to its business model. Even if Kodak had embraced digital technology, wouldn’t they have still had to lay off tens of thousands of people in the process? Wouldn’t they have had to stop making film, printing paper, and doing all of those tasks on which they had built a 90% market share? The Kodak of my childhood, the one that paid for my college education, gave a canvas for Hollywood’s imagination, and inspired Paul Simon to write one of my favorite songs, that Kodak had to disappear because something better came along.
It used to be that photography was a mysterious process to most consumers. They bought film from Kodak without understanding how it worked. Kodak succeeded by making the process easy enough for the average person to do. People used the camera without knowing how their pictures would turn out, sent the film off to get it magically transformed into photographs that they could show others. Ironically, the company that literally made black boxes made billions by keeping the process a black box for most people. Then came digital photography, cameras on phones, and eventually social media. Now there was no need for film, no need for cameras, no place to send the photos to get developed, and even no need to be on the same continent to share pictures with people. Technology eviscerated Kodak’s business model by removing the black box. It wasn’t just digital cameras that doomed Kodak, making it easy to carry cameras everywhere and to share with people instantly was also needed…
Dr. Rob proceeds to apply this lesson to the idea of health care reform:
Health care has previously been a black box to most consumers – a mysterious process by which the high priests (doctors) would perform healing through the use of their special knowledge and the wondrous healing of medications. But unlike Kodak, health care was able to keep raising prices instead of becoming more efficient. Now the health care industry has an economy larger than nearly all countries on this planet. The number of people employed by this economy is staggering, and the number of businesses built off of this model of inefficiency is huge. Imagine the damage an “Instagram of health care” could cause.
That is why I no longer feel that the solution to our problem will come from within the system: the system itself must be eviscerated for it to survive, and most systems (like Kodak) don’t see evisceration as a good business strategy. Legislators may pretend to pursue meaningful reform, but far too many of their constituents stand to lose their jobs if they succeeded, and far too much of their campaign funds come from companies built on the old economy of waste. Having hospitals oversee ACO’s [Accountable Care Organizations] is like putting Kodak executives in charge of laws concerning digital image sharing.
So what would the “Instagram of health care” look like? I think it would:
- Rely on technology to simplify things greatly.
- Use social technology to cut out black boxes.
- Put the control of care in the hands of the people who use it.
In a tiny, little way, this is what my informal Facebook Focus Group experiment is pointing me towards. Why not try to step out of the system (before it is eviscerated anyway) and at least try to do things in a new way.
(photo: Kodak No. 2A Brownie (Model C) by flickr user John Kratz)
The Doctor will E you now…
In my Facebook Focus Group experiment, one of the leading concerns was decreasing wait times in the office. Many people expressed dissatisfaction with taking an hour off from work, waiting an hour in the waiting room, and 30 minutes in the exam room (missing more work than planned), and then spending only 7 minutes in front of the physician for a simple problem. And who can blame them?
Another (single) response suggested e-visits. What’s an e-visit, you say? An e-visit is an encounter with a doctor or a nurse that doesn’t involve a trip to the office. It might be by phone or by teleconference. Sometimes it involves a pre-visit questionnaire. You don’t hear a lot about e-visits because, like so many things we do, it all depends on what the insurance companies think about it. If the health insurance companies in an an area pay for e-visits (and they do in some places, typically at discounted rates), then patients usually are excited to take advantage of them. Typically for simple problems or follow up for ongoing management of stable, uncomplicated chronic disease states.
Assuming reimbursement is not an issue, are they okay? Can a doctor do as good a job without seeing a patient face-to-face? A new study was just published that looked at simple problems like UTI’s and sinus infections found e-visits to be more cost effective and similarly effective. The one difference they found was that those receiving care in an e-visit were more likely to receive antibiotics then those seen in person. But there was no ultimate difference in outcomes.
My opinion is that, when your doctor knows you well, a lot of what typically happens in the office could safely happen over the phone (or via teleconference), and certainly be more convenient for the patient, compared to taking time off work and suffering long waits in the office. I’m interested to know how you feel…
Shoot for the Moon. And Bacon.

I posted the following status update on Facebook today and had an overwhelming 180-plus responses, and dozens of “likes” endorsing individual answers. It was amazing. Although not very scientific, the exercise turned out to be a good marketing survey!
Facebook Focus Group time–Other than a doctor that knows what he or she is doing, what do you want in a doctor’s office? Shoot for the moon. Do you want free lollipops? Evening hours? Humans answering the phones? Reply with one or three things you think you would want from your doctor?
(Please comment here whether or not you have been a patient of mine in the past, or whether you want to be in the future. This is for anyone who has ever been a patient. Forget what is conventionally available. Ask for anything you want!)
My purpose is obvious. I am hoping to start a new practice on Nantucket, and need to decide on what I want that practice to look like. What better way to plan it than to ask the people it might matter to the most?
In asking everyone to “shoot for the moon,” I wanted honest opinions about how an office should run, about what would make a new practice stand out, and be the best one out there.
Here are the results. I grouped the responses into categories and summed their mentions and “likes.” In order:
40 Online access to medical records
35 Decreased wait times
31 Dual waiting rooms—sick and well
31 Undivided attention/good listening
27 Evening hours
27 Weekend hours
25 Attention to diet/nutrition/exercise, overall wellness
24 Email access
21 Help to avoid unnecessary ER visits
18 Questions to prompt for reasons for visit (during visit or before)
18 Courtesy call if running late
18 Courtesy from receptionist
18 Avoid triage or gatekeeper role of receptionist
17 Alternative/integrative treatment options
16 Online self-scheduling tool
15 Waiting room comfort (seating, temperature, good magazines, privacy)
15 Decreased wait for appointments
12 No automated answering machines
10 Bacon
10 Followup with test results
9 Comfortable exam room environment (seating, lighting, good magazines)
9 Seeing doctor, not NP or PA
8 Walk-in slots
8 Enhanced check-in technologies
8 Respect my opinions on illness
7 Donuts
7 Alerts/reminders from doctor
6 Telephone access for after-hours emergencies
5 Coffee
4 Teleconference (Skypelike) or other alternative visit options
4 Nutella
4 Wifi
3 No lollipops
2 Lollipops
2 Home-cooked meals
1 Same day appointments
1 Cookies
1 Snacks
1 Drinks
1 “Fancy” chocolates
1 Massages
Pretty interesting results, don’t you think? First of all, it would seem that it is more important for me to provide complimentary bacon to my patients than a comfortable exam room environment or walk-in slots for appointments. Why didn’t I think of that? Bacon is always the key to excellent customer service!
You can tell the thread had a little humor in it, and that is always a good thing. But, ignoring the requests for Nutella and home-cooked meals, I was happy to see that online access to medical records was the most “liked” topic. This shouldn’t be a surprise. Today’s patients, raised on WebMD and the University of Google want to be involved in their care, or at least feel well-informed about their visits.
In October, a study was published in the Annals of Internal Medicine that looked at the interaction between clinician and patients (as well as the satisfaction each party feels and its affect on healthcare) when visit notes were made available after every doctor’s visit. It was summarized as follows in an article on the study in Forbes magazine:
“Patients accessed visit notes frequently, a large majority reported clinically relevant benefits and minimal concerns, and virtually all (99%) patients wanted the practice to continue. With doctors experiencing no more than a modest effect on their work lives, open notes seem worthy of widespread adoption.”
So now, in my own little study, my Facebook friends have put online access to medical records as their number one request in an “ideal medical practice.” In the study, this meant actually delivering copies of the notes. But there are different ways to interpret this informal request from Facebook, especially since I did not specify what this would entail. Other than in the study environment described above, not many electronic medical records are programmed to share visit notes online, as this is something that, prior to this study, is so foreign to ambulatory medicine that it has likely never been requested of the health IT companies. Today, online access to medical records is more likely to be represented in a patient portal, written by the software companies, to which a patient can securely log in and see some portion of their records. This should, in the least, include appointment requests, problem lists, allergies, medicine list, visit summaries, lab results, and secure messaging.
“Decreased wait times” is not a surprise at number two, given our severe doctor shortage and the pressures from our third-party payer system that makes a doctor see more and more patients each day to maintain a steady income. If I were to recreate the practice that I left, the mill that grinded me up and spit me out in a bag of grits, I would have the same situation all over again. In opening a new practice, I will need to find a way to limit the overall patient load to better match the advanced level of service I am talking about trying to provide, which includes minimal wait times. I think at least part of the solution, in addition to limiting patient load, is found farther down the list. If I try to mostly stick to same day scheduling, allowing patients to schedule their own appointments online, and offer alternative visit options like Skype or telephone visits, then I should be able to limit the time spent waiting for me to see you.
Coincidentally, this will also help me take care of the issue that surprised me by coming in third, having a dual waiting room, separating the sick from the well. Going forward, I do not want a practice with more than one person waiting!
So what is next? I need to take this list, as grandiose as it may seem, and see if I can come up with a practice model that can make it happen. I am going to try!